 
These include manual lymphatic drainage, compression garments, and self massage. This can be done by a therapist, a caregiver, or the person.Īlso, it has been observed in studies that better results in swelling reduction were achieved when the compression pump was combined with other therapies. Lymphedema pumps work great when used correctly, and in conjunction with other approaches.įirstly, it is recommended that manual lymph drainage is performed first to prepare the lymphatic system to receive the lymph fluid. The body can then process the fluid normally. In the case of someone experiencing lymphedema, this is used to move the lymph fluid from the affected limb, with the aim of reducing swelling.įor example in lower limb lymphedema such a device can be used to move the fluid back up to the functioning lymph nodes located in the groin. The chambers then deflate, and can be set to inflate/deflate at different intervals and patterns, hence the name intermittent pneumatic compression. The device has sleeves containing several chambers, which inflate to apply pressure to the limb the device is fitted to. What Are Sequential Compression Devices For Lymphedema?Ī sequential compression device for lymphedema is used to deliver intermittent pneumatic compression (IPC). Hopefully this will leave you better informed before deciding on this type of treatment for lymphedema. In this article we will take a closer look at the evidence for using compression pumps (aka sequential compression devices) for lymphedema. 2006 81:17-27.The use of compression pumps for lymphedema has a long history.Īnd depending on who you ask, you will get differing opinions on whether these pumps are good or bad for lymphedema. Ropinirole in the treatment of patients with restless legs syndrome: a US-based randomized, double-blind, placebo-controlled clinical trial. 2004 13:679-693.īogan RK, Fry JM, Schmidt MH, Carson SW, Ritchie SY. Validation of the Restless Legs Syndrome-Quality of Life Instrument (RLS-QLI): findings of a consortium of national experts and the RLS foundation. 2003 4:101-119.Ītkinson MJ, Allen RP, DuChane J, Murray C, Kushida C, Roth T. Restless legs syndrome: diagnostic criteria, special considerations, and epidemiology. 
2001 56:263-265.Īllen RP, Picchietti D, Hening WA, Trenkwalder C, Walters AS, Montplaisir J. MRI measurement of brain iron in patients with restless legs syndrome. 2003 106:23-27.Īllen RP, Barker PB, Wehrl F, Song HK, Earley CJ. Iron deficiency anemia and restless legs syndrome: is there an electrophysiological abnormality? Clin Neurol Neurosurg. In this group of patients, wearing the SCD in the evening for an hour improved symptoms of RLS and improved quality of life, with complete resolution of symptoms in 3 of 10 patients.Īkyol A, Kiylioglu N, Kadikoylu G, Bolaman AZ, Ozgel N. Every quality of life score improved: social function from 74% to 96% (p = 0.04), daily task function 63% to 80% (p = 0.05), sleep quality 27% to 63% (p = 0.003), and emotional well-being from 49% to 83% (p = 0.02). Epworth Sleepiness Scale score improved from 12/24 to 8/24 (p = 0.05). Group severity score improved from 24/40 to 8/40 (p = 0.001). Three patients experienced complete resolution of RLS and 6 patients had improvement of symptoms. The remaining 9 patients complied with therapy 58%-100% of nights (mean, 82%). Of 10 patients (7 women age range, 37-80 yr mean age, 56 yr), symptomatic for a mean of 68 months (range, 12-360 mo), 1 could not tolerate wearing the SCD and withdrew from the protocol after 3 days. Compliance with SCD therapy was measured using patient-recorded logs. Before and after 1-3 months of SCD therapy, patients completed validated questionnaires to assess RLS severity, daytime sleepiness, and impact of RLS on quality of life in the domains of social function, daily task function, sleep quality, and emotional well-being. 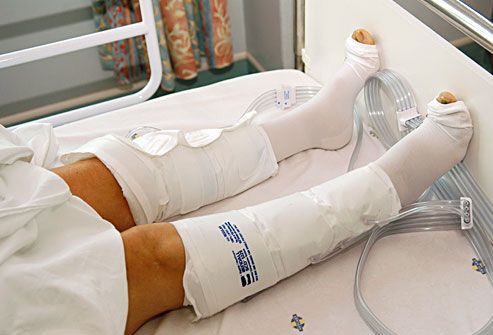
Patients were asked to wear the SCD for an hour each evening before the usual time of onset of restless legs symptoms. We performed an uncontrolled, prospective interventional study using SCDs on a convenience sample of adults reliably diagnosed with RLS. The objective of this study was to determine the therapeutic effect of pneumatic sequential compression devices (SCDs) on RLS symptoms. 
Here we review RLS and its treatment and present data from a pilot study on the effect of a novel treatment for this condition. An effective nonpharmacologic therapy would be highly desirable. Treatment of first choice for RLS is usually medication, but medications are often ineffective or poorly tolerated. RLS commonly causes insomnia and associated daytime symptoms. Restless legs syndrome (RLS) is a common disorder that presents with irresistible urges to move the legs and motor restlessness, worsening in the evening. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
